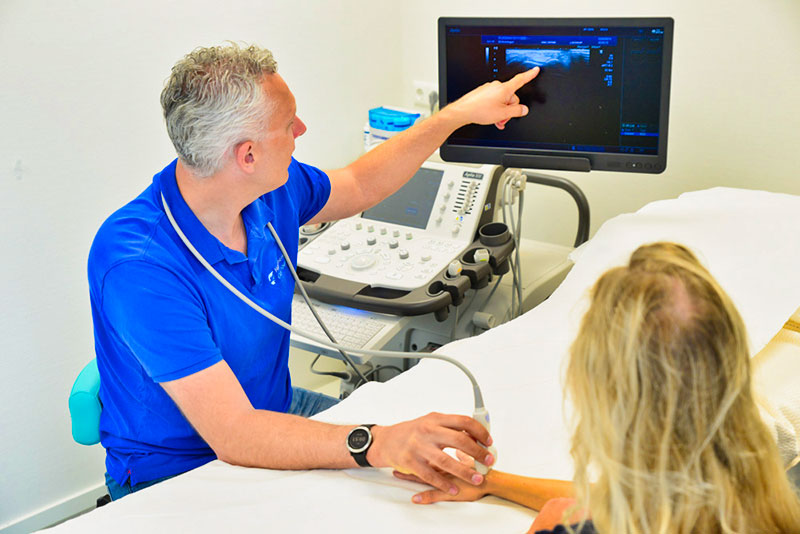
Er zijn in Nederland zo’n 10.000 klimmers, waarvan 75% wel eens te maken heeft gehad met klachten aan de hand, pols of arm. Klimmers belasten hun handen ontzettend zwaar, waardoor ze snel te maken krijgen met blessures. Veelvoorkomende handblessures bij klimmers zijn:
Partiële of complete ruptuur van een pulley.
Hierbij scheurt er een bandje dat dwars over de pees loopt, we hebben hier meerdere van. Wanneer dit gebeurt bemerk je meestal een knapje tijdens het klimmen, waarna er pijn ontstaat aan de handpalm zijde van de vinger. Wanneer de pulley, ook wel ringbandje genoemd, scheurt bij een tenduegreep (open greep) ontstaat de pijn vaak tussen het middelste en het laatste gewricht van de vinger. Bij een arqué (crimp) is dit iets lager, onder het middelste gewricht van de vinger.
De behandeling hangt af van de ma te van beschadiging van de pulley, dit is goed te zien op een echo. Deze kunnen wij zelf op de praktijk maken.
te van beschadiging van de pulley, dit is goed te zien op een echo. Deze kunnen wij zelf op de praktijk maken.
Wanneer één of meerdere bandjes gescheurd zijn leren we je een tapetechniek en krijg je in sommige gevallen een beschermring. Daarnaast krijg je na 2-4 weken rust een oefenprogramma waarbij je heel geleidelijk de pezen en bandjes weer mag belasten. Mathieu Ceron (trainer en fysiotherapeut van het Nederlands klim- en boulderteam) heeft dit programma ontwikkeld. Op zijn website deklim.site vind je meer informatie over klimmen en klimblessures.
Overbelasting van de buigpezen van de vingers.
Wanneer de peesschede geïrriteerd is door de zware belasting noemen we dit tendovaginitis van de flexorpezen. In de volksmond wordt vaak gesproken over een ‘klimvinger.’
Heel anders dan bij een pulleyruptuur ontstaan deze klachten geleidelijk. Deze pezen aan de binnenzijde van de vingers kunnen zwellen en het maken van een vuist kan pijnlijk zijn. Ook kunnen de buigpezen gevoelig zijn wanneer erop gedrukt wordt. Rust is de beste oplossing hiervoor en het aanpassen van je klimtechniek kan helpen bij het herstel. Soms wordt er een injectie gegeven met een ontstekingsremmend middel.
Wanneer er een nodus (bultje) in de pees ontstaat kan het zijn dat je vinger gaat hokken, we spreken dan van een triggerfinger,je voelt dan een verdikking in de handpalm. Je leest hier meer over onder het kopje triggerfinger.
Het scheuren van een intrinsieke handspier.
Wanneer je aan één vinger hangt en je voelt een knapje dan kan het zijn dat één van de intrinsieke handspieren verrekt of gescheurd is. We noemen dit een lumbrical tear of shift. Ook dit is op een echo goed te diagnosticeren, je wordt behandeld met tape en mag 2-4 maanden geen greep meer doen met één vinger.
Elleboogblessures
Hoewel handblessures het de meest problemen geven bij klimmers, staan elleboogblessures op een goede tweede plaats. Veelvoorkomend zijn epicondylitis lateralis; een overbelastingsprobleem van de strekkers van de pols en vingers, deze hechten aan op de buitenzijde van de elleboog. Daarnaast komt epicondylitis medialis ook veel voor, dit is een irritatie van de binnenzijde van de elleboog, hier hechten de polsbuigers en vingerbuigers aan. Ook voor deze elleboogklachten kunt u bij ons terecht.

 Op de afbeelding ziet u de test van Finkelstein, wanneer deze erg pijnlijk is (pijnlijker dan aan de niet aangedane zijde) kan het zijn dat u de aandoening van Quervain heeft.
Op de afbeelding ziet u de test van Finkelstein, wanneer deze erg pijnlijk is (pijnlijker dan aan de niet aangedane zijde) kan het zijn dat u de aandoening van Quervain heeft.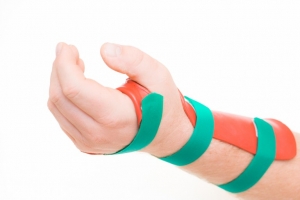 Verder kunnen we u adviezen geven om de zenuw zo min mogelijk te irriteren bij uw dagelijkse bezigheden. Soms helpt dit, wanneer het niet helpt verwijzen we u terug naar de huisarts, deze kan een injectie geven of u verwijzen naar het ziekenhuis. Hier wordt dan gekeken of u in aanmerking komt voor een operatie.
Verder kunnen we u adviezen geven om de zenuw zo min mogelijk te irriteren bij uw dagelijkse bezigheden. Soms helpt dit, wanneer het niet helpt verwijzen we u terug naar de huisarts, deze kan een injectie geven of u verwijzen naar het ziekenhuis. Hier wordt dan gekeken of u in aanmerking komt voor een operatie. Soms wordt er gekozen voor een beschermende spalk, waarin u op eigen kracht binnen 5 dagen na de operatie weer mag gaan bewegen. U krijgt dan oefeningen waarmee u zonder veel kracht alweer kunt gaan oefenen met de geopereerde vingers, uiteraard begeleiden wij u hier intensief in.
Soms wordt er gekozen voor een beschermende spalk, waarin u op eigen kracht binnen 5 dagen na de operatie weer mag gaan bewegen. U krijgt dan oefeningen waarmee u zonder veel kracht alweer kunt gaan oefenen met de geopereerde vingers, uiteraard begeleiden wij u hier intensief in. Handtherapeutische behandeling
Handtherapeutische behandeling Na drie weken gaan we het aangedane gewricht opnieuw onderzoeken. Wanneer deze stabiel is hoeft u het spalkje niet meer te dragen, u krijgt dan oefeningen om de bewegelijkheid te onderhouden. Wanneer uw vinger erg stijf geworden is, krijgt u een nieuw spalkje, nu juist om het strekken te verbeteren. Wanneer het gewricht nog steeds instabiel is, adviseren we u om het spalkje dat het strekken beperkt nog een week of een aantal weken te dragen, we blijven het herstel monitoren.
Na drie weken gaan we het aangedane gewricht opnieuw onderzoeken. Wanneer deze stabiel is hoeft u het spalkje niet meer te dragen, u krijgt dan oefeningen om de bewegelijkheid te onderhouden. Wanneer uw vinger erg stijf geworden is, krijgt u een nieuw spalkje, nu juist om het strekken te verbeteren. Wanneer het gewricht nog steeds instabiel is, adviseren we u om het spalkje dat het strekken beperkt nog een week of een aantal weken te dragen, we blijven het herstel monitoren.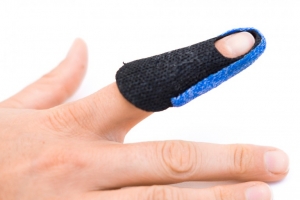 Soms worden er kant en klare spalkjes voorgeschreven, vaak gaat dit irriteren op de huid. Ook staat het topje hier niet altijd recht genoeg in, de pasvorm is dan niet goed. Dit is de reden dat wij er de voorkeur aan geven om deze op maat voor u te maken.
Soms worden er kant en klare spalkjes voorgeschreven, vaak gaat dit irriteren op de huid. Ook staat het topje hier niet altijd recht genoeg in, de pasvorm is dan niet goed. Dit is de reden dat wij er de voorkeur aan geven om deze op maat voor u te maken. Wanneer de artrose in een vergevorderd stadium is kunt u hieraan geopereerd worden. Na de operatie kunt u weer bij ons terecht om de hand en pols weer soepel en sterk te krijgen.
Wanneer de artrose in een vergevorderd stadium is kunt u hieraan geopereerd worden. Na de operatie kunt u weer bij ons terecht om de hand en pols weer soepel en sterk te krijgen. Daarnaast geven we uw oefeningen mee, deze zijn erop gericht om de spierbalans in uw hand te herstellen. Deze is bij reuma namelijk vaak verstoord. Ook zijn de oefeningen gericht op het ontspannen van de hand.
Daarnaast geven we uw oefeningen mee, deze zijn erop gericht om de spierbalans in uw hand te herstellen. Deze is bij reuma namelijk vaak verstoord. Ook zijn de oefeningen gericht op het ontspannen van de hand.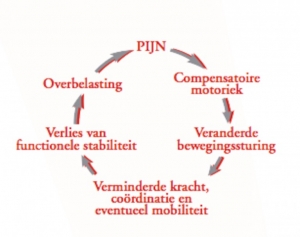 bron: Oefentherapie voor chronische onbegrepen polsklachten door: A.J. Videler, M. Kreulen, M.J.P.F. Ritt
bron: Oefentherapie voor chronische onbegrepen polsklachten door: A.J. Videler, M. Kreulen, M.J.P.F. Ritt Handtherapeutische behandeling
Handtherapeutische behandeling Handtherapeutische behandeling
Handtherapeutische behandeling te van beschadiging van de pulley, dit is goed te zien op een echo. Deze kunnen wij zelf op de praktijk maken.
te van beschadiging van de pulley, dit is goed te zien op een echo. Deze kunnen wij zelf op de praktijk maken.